For physicians, this is routine and uncomplicated surgery. For the families of ailing seniors, it is yet another medical procedure fraught with uncertainty that arouses disturbing questions and fears about life and death, often accompanied by feelings of guilt and family turmoil.
Little controversy surrounds the use of percutaneous endoscopic gastronomy (PEG) tubes in patients with long-term nutritional needs but good prospects for recovery from whatever condition has interfered with their ability to eat.
No one can point to a single culprit or clear explanation for why the medical profession continues the controversial and routine practice of surgically implanting feeding tubes in the stomachs of dying, elderly patients.
But a lot of people in the healthcare industry are reaping the benefits. Like hospitals. And nursing homes. And the global medical technology giants.
Feeding tubes surgically implanted into the stomach are coming under growing criticism in medical care for the elderly, even as their use among the frail, terminally ill and often demented patients has become commonplace.
The majority of these patients are dying from progressive neurological diseases like Alzheimer’s, but physicians continue recommending the surgery to people despite lack of solid medical evidence that patients will benefit. Moreover, experts say tube feeding in such situations may do more harm than good.

“It’s not a benign procedure,” said Dr. David Weissman, a palliative care physician and professor emeritus at the Medical College of Wisconsin in Milwaukee.
It potentially has serious consequences on patients’ health and emotional states. Even if the surgery goes smoothly, as it typically does, it has risks, such as uncontrolled bleeding in the stomach, inflammation or infection and inhaling contents of the stomach into the lungs.
And the tubes, which protrude from their stomachs, often diminish patients’ quality of life, cause emotional distress and adversely affect their sense of dignity and humanity. For families of patients who have lost the ability to provide an informed consent, the decision to let a doctor insert the tube in their loved one often becomes a wrenchingly divisive issue.
“The insistence on such interventions approaches what I consider [going] against one of the tenets of medicine, and that is do no harm,” said Dr. Timothy Ihrig, a Des Moines physician specializing in palliative care. Palliative care is a branch of medicine focusing on relieving pain and suffering and improving the quality of life for people facing the pain, symptoms and stresses of serious illness.
Despite a decade of research casting doubt on the practice, critics say medical professionals order the tubes when not medically necessary as a matter of routine. They do it to appease distraught family members and to avoid in-depth conversations about dying loved ones, or as a way of hastening discharge of the patient from the hospital and reducing expenses. Dependence on PEGs is also wrapped up in the complex economics of healthcare and the fact that people live longer.
Table of Contents
ToggleInvented for The Young, Used for The Elderly
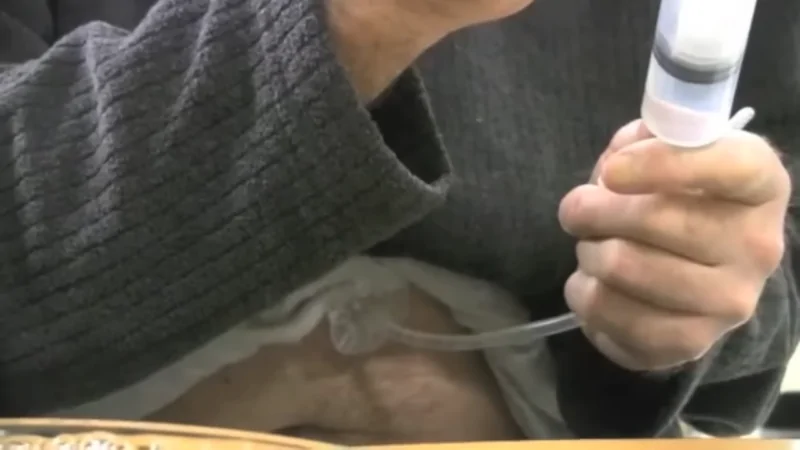
At issue is the PEG tube – standing for percutaneous endoscopic gastrostomy.
They first came into use in the 1980s to provide nutrition for children and young adults unable to eat. They introduced an important technological advance over intravenous nutrition or more difficult stomach surgeries.
Costing around $3,000 to implant, the device is considered particularly useful for patients with certain kinds of cancers, digestive disorders and burns. PEG tubes have important and even life-saving uses among younger patients and others who can benefit.
Questions about the proper use of feeding tubes gained national attention in the case of Terri Schiavo, a Florida woman who suffered severe brain damage on Feb. 25, 1990, that left her in a vegetative state at age 26. Schiavo’s husband and her parents battled each other in the courts for her last seven years, until the husband’s wish to have the tube removed finally prevailed in 2005, but not before the dispute had roiled Congress and reached the White House.
Today, the controversy is not just about an individual case or those in a vegetative state. However, it touches on some similar emotional and cultural issues surrounding modern medical care.
The focus is the widespread and routine adaptation of the PEG tube for patients in the nation’s burgeoning senior population despite many questions about the practice, especially when used in weak elderly patients, including some with advanced dementia. The elderly are now the main clientele for PEG tubes.
PEG tube insertion in the U.S. has more than tripled over the past two decades, an increase coinciding with the rise in the elderly population.
In 1988, around 60,000 PEG tubes were used on patients 65 years and older on Medicare. For the year 2004, the number reached nearly 150,000. The October 2010 issue of the medical journal Nutrition in Clinical Practice estimated that 188,000 PEG tubes had been placed in Medicare patients so far that year, a rate that was on pace to eventually quadruple the 1988 figure.
In Iowa, PEG procedures also have been on the rise, but at a slower rate over the past dozen years. PEG placements rose from 1,032 in 1997 to a high of 1,365 in 2008, with a slight decrease in 2009-2010, according to the best available data from the Iowa Hospital Association.
On average, patients aged 65 and over represented about 61 percent of those receiving the procedure, but a growing proportion are aged 45-64. Children and infants, for whom the technique was developed, are now a small minority of recipients.
The Tube-Feeding Death Spiral

Critics of routine PEG implantation in elderly patients are found among physicians, nurses, social workers, speech pathologists and others, and some fear that without concerted attention to the method’s drawbacks, the trend will pick up speed as the affected population grows.
The most recent U.S. census counts 40.3 million Americans aged 65 and older as of April 2010, a rise of about 15 percent from 2000, while the nation’s population as a whole grew by 9.7 percent. The aging of post-World War II baby boomers will only accentuate this trajectory.
Weissman, the Wisconsin physician, outlines a typical scenario that he calls “the tube-feeding death spiral” related to routine use of PEGs for patients with chronic, debilitating neurological diseases:
- A patient nearing the end of a fatal chronic illness is admitted to the hospital for an acute medical problem.
- Medical staff observe that the patient is swallowing with difficulty, losing weight, or inhaling food and drink.
- A doctor orders a swallow study, leading to a recommendation that the patient receive “non-oral feeding” out of concern the person will choke or not eat enough.
- The feeding tube provokes “agitation.” Sometimes the patient is transferred to a more secure care facility. If not, the patient’s distress dislodges the feeding tube.
- The tube is reinserted, and the patient’s hands or chest are tied down.
- The patient chokes on his or her own body fluids and develops pneumonia.
- The patient gets antibiotics through an IV, and a sensor clipped to a fingertip, earlobe or toe monitors the amount of oxygen in the blood, a method called pulse oximetry.
- The tube might fall out and be replaced several times before a family conference is finally convened to discuss what to do.
- The patient dies.
“We see this all the time in the hospital,” Weissman said.
The American Gastroenterological Association recommends the PEG tube for feeding patients who cannot or will not eat and require more than a temporary remedy. The association also says patients who undergo the surgery must have functioning digestion and be able to tolerate the operation.
But people with Alzheimer’s or other neurological illnesses, even if they meet these qualifications, are not necessarily going to benefit from a PEG. There is no proof that feeding patients dying from neurological illnesses with prepared formulas pumped through stomach tubes enhances either length or quality of life.
As their symptoms worsen, such patients commonly lose their appetite or the motor skills required to eat. They also may have difficulty swallowing, putting them in danger of inhaling food or liquids into the lungs, known as aspiration, which can cause life-threatening pneumonia.
PEG Won’t Reduce Dying Process

For those nearing life’s end, inserting a feeding tube doesn’t reverse the process of dying, said Dr. John Rachow, a University of Iowa Hospital and Clinics geriatrics specialist. The ability to eat is often the last function to go before patients with advanced dementia die; it is “the clinical marker of their terminal state,” as Rachow puts it. At this stage, a feeding tube becomes “a pointless intervention,” he said.
Or worse than pointless, according to Weissman, the Wisconsin doctor.
Confused elderly patients may be alarmed to find a tube protruding from their stomach, Weissman said; some have to be physically restrained so they won’t pull the tube out.
Furthermore, PEG tubes don’t always ward off the problems they are supposed to prevent – such as keeping patients with advanced dementia from getting aspiration pneumonia. “Putting in a feeding tube does nothing to prevent aspiration,” Weissman said.
This is because people who can’t swallow still may inhale their own saliva or gastric juices from the stomach into the lungs, which is no less dangerous than breathing in food and drink.
Des Moines physician Timothy Ihrig thinks unnecessary PEG tubes are not only unethical, but also wasteful. “I’ve seen times where tubes have been put in and the patient pulls them out, but it keeps going back in,” he said. “It’s not open heart surgery. But if someone is going to gain nothing from it, then why do it?”
Making the Feeding Tube Decision

At the University of Iowa’s hospital, the state’s largest hospital and only academic medical center, annual PEG insertions more than doubled between 2003 and 2008, going from 121 to 296. The number has fallen since the peak year of 2008, with 224 tubes placed in 2009 and 233 in 2010. The number of total discharges also increased over those eight years, but at a much lower rate.
Although Iowa still has one of the lowest rates of PEG tube insertions in the country – a 2009 Brown University study found the state had the fourth lowest rate nationwide –some doctors nevertheless are dismayed by what they are seeing.
Rachow, as attending physician for numerous nursing homes in southeast Iowa, said he’s witnessed an increase over the past decade in the number of patients coming to nursing homes with a PEG tube in place after short hospital stays, even when a long-term feeding device seems unwarranted. “The more it’s done, the more it just becomes the standard,” he said.
The American Gastroenterological Association says patients who are not eating normally should start getting nourishment within one to two weeks after admission to the hospital, and recommends the PEG for patients who need feedings by tube for more than 30 days.
The University of Iowa Hospital and Clinics makes the decision faster: If a patient’s ability to eat has not improved within 48 to 72 hours, the healthcare team begins to consider strategies on how to feed the patient, according to Dr. Justin Smock, an internal medicine clinician.
“Nutrition is critically important for improvement in getting over illness,” he said.
Swallowing Difficulty Major Issue
In considering whether to place a PEG tube, the possibility that eating by mouth might lead to a patient’s death weighs heavily on the minds of physicians. Doctors may order a swallow test, overseen by a speech pathologist. Mild swallowing problems might call for simply a change in diet, while severe swallowing problems may result in a feeding tube, which requires a doctor’s order and the patient or family’s consent.
“Once we know the patient needs a PEG tube, the hospital is pretty good about getting them in,” said Molly Klokkenga, a social worker in the UI Hospital neurology unit. “If physical or occupational therapy says they need skilled [care] and they’re having difficulty swallowing, then we’ll just go ahead and do a PEG tube.”
Smock said swallow studies “almost always confirm what you know,” and geriatrician Rachow agreed. However, he cautioned against relying on swallow tests when abnormal swallowing may be a temporary condition apart from underlying chronic problems. “There’s a flaw in the logic that a swallowing test during acute illness really tells you what they had before they got sick,” he said.
In Rachow’s view, the swallow test can become a means for physicians to justify the insertion of a PEG tube in the context of intense anxiety. Patients and their families typically face great uncertainty about the kind of care that will follow a hospital stay, and by placing a PEG, doctors help relieve their anxieties, he said.
Rachow wishes more physicians would call him before their patients go to nursing homes, but most do not: He said he hears from doctors in about one out of five cases. Medical residents who often handle discharges are especially busy, he noted. “A lot of pressure is on them to move the patient through. The young doctor in an internship, buried in work, just can’t see that there is another world of care going on outside the hospital.















